According to Koen Leurs, professor of gender, media and migration studies at Utrecht University in the Netherlands, we have arrived at a point where migration management has become so reliant on digital technology that the former can no longer be studied in isolation from the latter. Investigating this reliance for his new book, Digital Migration, Leurs came to the conclusion that applications like those mentioned above are more often than not a double-edged sword, presenting both benefits and drawbacks.
There has been “a huge acceleration” in the way digital technologies “dehumanize people,” says Koen Leurs, professor of gender, media and migration studies at Utrecht University in the Netherlands. Governments treat asylum seekers as test subjects for new inventions, all along the borders of the developed world.
On the one hand, digital technology can make migration management more efficient and less labor intensive, enabling countries to process larger numbers of people in a time when global movement is on the rise due to globalization and political instability. Leurs also discovered that informal knowledge networks such as Informed Immigrant, an online resource that connects migrants to social workers and community organizers, have positively impacted the lives of their users. The same, Leurs notes, is true of platforms like Twitter, Facebook, and WhatsApp, all of which migrants use to stay in touch with each other as well as their families back home. “The emotional support you receive through social media is something we all came to appreciate during the COVID pandemic,” Leurs says. “For refugees, this had already been common knowledge for years.”
On the flipside, automatization of migration management – particularly through the use of AI – has spawned extensive criticism from human rights activists. Sharing their sentiment, Leurs attests that many so-called innovations are making life harder for migrants, not easier. He also says there has been “a huge acceleration” in the way digital technologies “dehumanize people,” and that governments treat asylum seekers as test subjects for new inventions, all along the borders of the developed world.
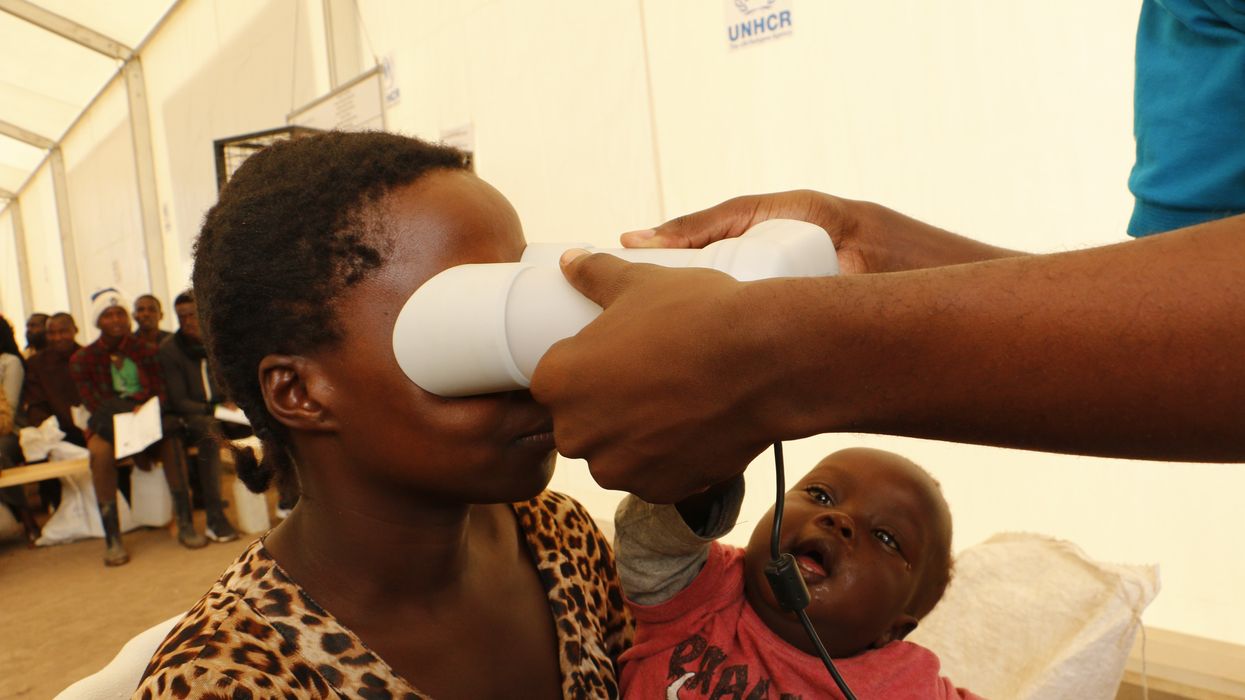
In Jordan, for example, refugees had to scan their irises in order to collect aid, prompting the question of whether such measures are ethical. Speaking to Reuters, Petra Molnar, a fellow at Harvard University’s Berkman Klein Center for Internet and Society, said that she was troubled by the fact that this experiment was done on marginalized people. “The refugees are guinea pigs,” she said. “Imagine what would happen at your local grocery store if all of a sudden iris scanning became a thing,” she pointed out. “People would be up in arms. But somehow it is OK to do it in a refugee camp.”
Artificial intelligence programs have been scrutinized for their unreliability, their complex processing, thwarted by the race and gender biases picked up from training data. In 2019, a female reporter from The Intercepttested iBorderCtrl and, despite answering all questions truthfully, was accused by the machine of lying four out of 16 times. Had she been waiting at checkpoint on the Greek or Latvian border, she would have been flagged for additional screening – a measure that could jeopardize her chance of entry. Because of its biases, and the negative press that this attracted, iBorderCtrl did not move past its test phase.
While facial recognition caused problems on the European border, it was helpful in Ukraine, where programs like those developed by software company Clearview AI are used to spot Russian spies, identify dead soldiers, and check movement in and out of war zones.
In April 2021, not long after iBorderCtrl was shut down, the European Commission proposed the world’s first-ever legal framework for AI regulation: the Artificial Intelligence Act. The act, which is still being developed, promises to prevent potentially “harmful” AI practices from being used in migration management. In the most recent draft, approved by the European Parliament’s Liberties and Internal Market committees, the ban included emotion recognition systems (like iBorderCtrl), predictive policing systems (like EUMigraTool), and biometric categorization systems (like iris scanners). The act also stipulates that AI must be subject to strict oversight and accountability measures.
While some worry the AI Act is not comprehensive enough, others wonder if it is in fact going too far. Indeed, many proponents of machine learning argue that, by placing a categorical ban on certain systems, governments will thwart the development of potentially useful technology. While facial recognition caused problems on the European border, it was helpful in Ukraine, where programs like those developed by software company Clearview AI are used to spot Russian spies, identify dead soldiers, and check movement in and out of war zones.
Instead of flat-out banning AI, why not strive to make it more reliable? “One of the most compelling arguments against AI is that it is inherently biased,” says Vera Raposo, an assistant professor of law at NOVA University in Lisbon specializing in digital law. “In truth, AI itself is not biased; it becomes biased due to human influence. It seems that complete eradication of biases is unattainable, but mitigation is possible. We can strive to reduce biases by employing more comprehensive and unbiased data in AI training and encompassing a wider range of individuals. We can also work on developing less biased algorithms, although this is challenging given that coders, being human, inherently possess biases of their own.”
AI is most effective when it enhances human performance rather than replacing it.
Accessibility is another obstacle that needs to be overcome. Leurs points out that, in migration management, AI often functions as a “black box” because the migration officers operating it are unable to comprehend its complex decision-making process and thus unable to scrutinize its results. One solution to this problem is to have law enforcement work closely with AI experts. Alternatively, machine learning could be limited to gathering and summarizing information, leaving evaluation of that information to actual people.
Raposo agrees AI is most effective when it enhances human performance rather than replacing it. On the topic of transparency, she does note that making an AI that is both sophisticated and easy to understand is a little bit like having your cake and eating it too. “In numerous domains,” she explains, “we might need to accept a reduced level of explainability in exchange for a high degree of accuracy (assuming we cannot have both).” Using healthcare as an analogy, she adds that “some medications work in ways not fully understood by either doctors or pharma companies, yet persist due to demonstrated efficacy in clinical trials.”
Leurs believes digital technologies used in migration management can be improved through a push for more conscientious research. “Technology is a poison and a medicine for that poison,” he argues, which is why new tech should be developed with its potential applications in mind. “Ethics has become a major concern in recent years. Increasingly, and particularly in the study of forced migration, researchers are posing critical questions like ‘what happens with the data that is gathered?’ and ‘who will this harm?’” In some cases, Leurs thinks, that last question may need to be reversed: we should be thinking about how we can actively disarm oppressive structures. “After all, our work should align with the interests of the communities it is going to affect.”